Key takeaways:
- Start where the impact is obvious. Go after use cases like readmissions or missed follow-ups, where acting early actually changes outcomes.
- Get your data in shape before anything else. If the data is messy or delayed, even the best model won’t hold up.
- Don’t overthink build vs buy. Most teams land somewhere in between, using existing platforms and customizing where it really matters.
- Fit AI into how clinicians already work. If it shows up in the tools they use every day, adoption feels natural.
- Start small, prove it works, then expand. A focused pilot with clear results makes scaling a lot smoother later.
Instead of reacting only when complications arise, organizations are using AI for chronic disease management to continuously monitor high-risk cases and respond promptly. With healthcare data analytics and predictive analytics in chronic disease management, teams can identify risks earlier and intervene before conditions escalate.
With remote patient monitoring and AI-powered tracking systems, care no longer stops at hospital visits. It continues in real time.
What’s accelerating this shift is the rapid pace at which AI is moving into core healthcare operations. According to a 2026 outlook by Deloitte, over 80% of health system and health plan executives expect AI to deliver moderate-to-significant value across clinical and operational functions.
As a result, healthcare systems are investing in scalable, integrated AI solutions. In this blog, you’ll see how AI is creating real impact in managing chronic diseases, how teams are implementing it, and what it takes to scale effectively.
Build Compliant AI Systems for Healthcare Outcomes
Shift from reactive care to scalable, compliant AI-driven systems.
High-Impact AI Use Cases in Chronic Disease Management
If you sit with a care team for a day, the gap becomes obvious. Most of the real risk doesn’t show up during scheduled visits. It builds quietly in between. That’s where AI in chronic disease management is starting to change how things actually work on the ground.
Instead of adding more dashboards or alerts, the focus now is on giving teams timely, usable signals without slowing them down. Here’s where that’s happening in practice:
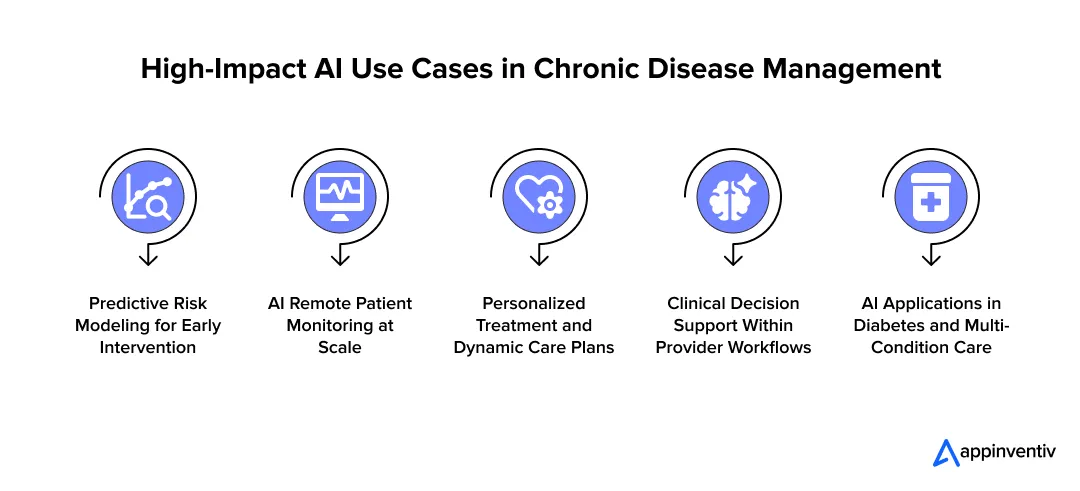
1. Predictive Risk Modeling for Early Intervention
This is usually the first place businesses start. The idea is simple: catch the problem before it turns into an admission.
- Combines EHR data, lab results, medication history, and patient behavior
- Uses predictive analytics in chronic disease management to flag high-risk patients early
- Helps care teams prioritize outreach instead of reacting late
- Reduces avoidable escalations and readmissions
In cardiovascular care, for example, deep learning models can detect irregular pulse patterns linked to atrial fibrillation with sensitivity levels reaching up to 98.3%, allowing teams to intervene much earlier.
In real settings, these models aren’t static. They’re updated regularly as patient data and patterns evolve.
2. AI Remote Patient Monitoring at Scale
Once a patient leaves the hospital, visibility drops. That’s been a long-standing issue.
- Uses IoT-based remote patient monitoring technology, like wearables and home devices
- Feeds continuous data into patient monitoring systems
- Identifies unusual patterns like sudden glucose spikes or irregular vitals
- Triggers alerts through AI remote patient monitoring solutions when something needs attention
This is especially relevant in respiratory care, where AI systems track lung function and environmental factors to predict asthma attacks or COPD flare-ups before they become critical. The value here isn’t just monitoring, but anticipating what’s likely to happen next.
The tricky part here isn’t collecting data. It’s filtering noise and making sure alerts are actually useful.
3. Personalized Treatment and Dynamic Care Plans
Chronic care isn’t one-size-fits-all. What works for one patient may not hold for another, even with the same diagnosis.
- Supports AI healthcare care management systems that adjust plans based on patient response
- Looks at adherence, lifestyle patterns, and treatment history
- Suggests small but meaningful changes before conditions worsen
- Scales chronic disease management AI solutions across large patient groups
You can already see this in conditions like diabetes and hypertension. AI-driven platforms use continuous glucose data to suggest insulin adjustments and meal changes in real time. In hypertension care, machine learning helps predict how patients respond to treatment, making medication decisions more precise. Recent studies show this leads to better treatment targeting, improved blood pressure control, and stronger patient adherence over time.
Over time, this shifts care from fixed plans to a more adaptive, responsive approach.
4. Clinical Decision Support Within Provider Workflows
If AI adds friction, it won’t get used. That’s why integration into daily workflows matters.
- Embeds insights into clinical decision support systems used during consultations
- Brings together structured records and unstructured notes
- Highlights risks, missed signals, or treatment gaps in real time
- Helps clinicians make faster calls without second-guessing data
The balance here is important. Too many alerts, and teams start ignoring them.
5. AI Applications in Diabetes and Multi-Condition Care
In reality, most patients have more than one condition. Diabetes, heart issues, and kidney problems often overlap.
- Uses AI applications in diabetes management for continuous glucose tracking and prediction
- Connects with AI patient monitoring apps for ongoing visibility
- Extends insights across conditions using AI chronic disease monitoring systems
- Supports coordinated care through integrated AI healthcare disease management systems
This is where things start to come together. Instead of treating conditions in isolation, systems begin to reflect the patient’s whole picture.
Step back and you’ll notice the shift. These aren’t standalone tools. They’re part of a broader move toward continuous, connected care, in which AI in chronic disease management helps teams stay ahead rather than constantly catching up.
Implementation Strategy for AI in Chronic Disease Management
When teams start thinking about AI, the first instinct is often to jump straight into tools or models. In practice, that rarely works. What makes the difference is how deliberately the system is put together, especially when you’re dealing with fragmented healthcare data and real clinical workflows.
Here’s how businesses are approaching AI in chronic disease management in a way that actually scales.
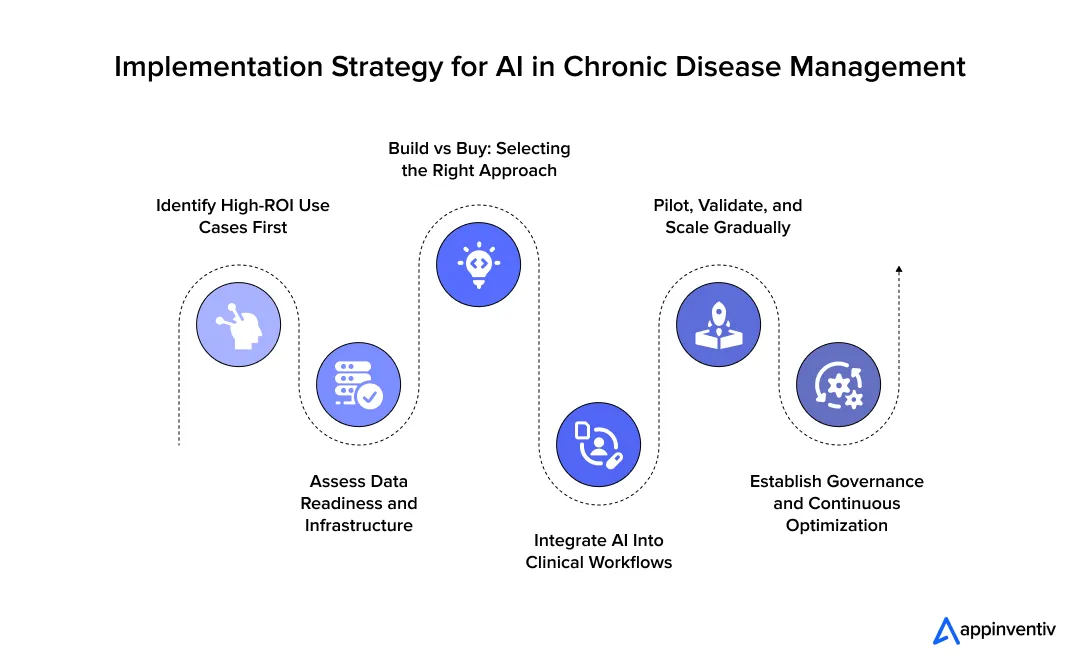
1. Identify High-ROI Use Cases First
Before anything gets built, the focus needs to be clear. Not every use case delivers the same value.
- Start with areas where delays directly affect outcomes, such as readmissions or missed follow-ups.
- Use baseline healthcare data analytics to understand where costs and inefficiencies are highest.
- Prioritize use cases where predictive analytics in chronic disease management can trigger early intervention
- Define success upfront, whether it’s reduced admissions, better adherence, or faster response times.
This step keeps AI for chronic disease management tied to real business and clinical impact rather than experimentation.
2. Assess Data Readiness and Infrastructure
Most challenges appear here, not the model itself.
- Audit data sources across EHRs, labs, devices, and patient apps
- Check for gaps, inconsistencies, and delays in data pipelines
- Normalize data using standard formats like FHIR, where possible
- Decide what needs real-time processing versus batch updates
For AI healthcare implementation in chronic care, clean, well-structured data matters more than model complexity.
3. Build vs Buy: Selecting the Right Approach
This is where many businesses lose time when decisions aren’t clear early on.
- Evaluate whether to build custom models or use existing platforms supported by AI Development Services.
- Consider integration effort, not just feature sets
- Look at how easily solutions plug into existing digital health platforms
- Assess vendor capabilities in handling AI remote patient monitoring solutions at scale
In most cases, a hybrid approach works best. Core systems are integrated, while specific capabilities are customized.
4. Integrate AI Into Clinical Workflows
Even the best model fails if it doesn’t fit into how clinicians work.
- Embed outputs directly into clinical decision support systems
- Surface insights inside existing dashboards, not separate tools
- Ensure alerts are contextual, not generic, to avoid fatigue
- Map outputs to clear actions, like scheduling follow-ups or adjusting care plans
This is what makes chronic disease management AI solutions usable, not just technically sound.
5. Pilot, Validate, and Scale Gradually
Going all-in too early usually creates friction.
- Start with a focused cohort, like a single condition or patient group
- Track performance using both clinical and operational metrics
- Monitor model accuracy, false positives, and missed signals
- Expand gradually across populations once results are stable
This phased approach helps build confidence in AI chronic disease monitoring systems before scaling.
6. Establish Governance and Continuous Optimization
AI systems don’t stay accurate on their own. They need ongoing oversight.
- Monitor model drift as patient populations and behaviors change
- Set up regular retraining cycles using updated datasets
- Define access controls and audit trails for sensitive patient data
- Align with compliance requirements while maintaining flexibility
Over time, this ensures AI healthcare disease management systems stay reliable and aligned with both clinical and regulatory expectations.
If you look closely, the pattern is consistent. Businesses that succeed with AI in chronic disease management don’t treat it as a one-time deployment. They treat it as a continuously evolving system, built on strong data foundations, integrated workflows, and clear outcomes from day one.
Appinventiv Insight
This is where most teams slow down. The strategy is clear, but getting it live across real systems is a different challenge. With 500+ digital health platforms and 75+ enterprise AI integrations, Appinventiv helps accelerate deployments by 30–40% and reduce implementation friction by up to 35%, without disrupting care workflows. A quick example makes this more concrete:
YouCOMM Health App
Challenge: Communication delays for speech-impaired patients.
Role: Built an AI-powered, real-time assistive communication app.
Impact:
- 0-delay patient-provider communication
- Fewer manual interventions
- Faster response in critical moments
Key Challenges in Adopting AI in Chronic Disease Management and How to Overcome Them
You usually notice these issues once things move beyond the pilot stage. Early results look promising, but day-to-day realities start to surface. The good part is that most of these challenges are familiar and can be handled upfront with the right setup.
| Challenge | What It Looks Like in Practice | How to Overcome It |
|---|---|---|
| Fragmented and inconsistent data | Data sits across EHRs, labs, and AI patient monitoring systems, often incomplete or not aligned | Put effort into data cleanup early. Validate inputs, remove duplicates, and standardize formats before relying on outputs |
| Low clinician adoption | Teams avoid new tools or ignore alerts because they don’t fit into existing workflows | Bring insights into systems they already use, like clinical decision support systems, and keep outputs simple and clear |
| Alert fatigue and noise | Too many alerts make it hard to tell what actually matters | Focus on fewer, high-value alerts using patient-specific thresholds instead of generic rules |
| Integration with legacy systems | Older systems struggle to connect with newer digital health platforms | Use healthcare APIs and middleware to bridge systems and ensure data flows without gaps |
| Data privacy and compliance concerns | Teams hesitate to scale due to regulatory risks around patient data | Set up encryption, role-based access, and audit logs from the beginning so compliance is built in |
| Model trust and explainability | Clinicians question outputs when there’s no clear reasoning behind them | Show supporting context with every insight so decisions feel grounded, not abstract |
| Scaling beyond pilot programs | What works in a small group doesn’t easily expand across the system | Start focused, track results closely, and scale step by step with proper governance in place |
When these are handled early, AI for chronic disease management feels less like a heavy rollout and more like a natural extension of how care is already delivered.
Fix What’s Slowing Your AI Scale-Up
If your AI initiatives are stuck at the pilot stage, the issue is rarely the model. It’s the system around it.
Key Benefits of AI in Chronic Disease Management
Spend some time with a care team a few months after rollout, and the difference shows up in small ways. The day feels a bit more under control. Fewer unexpected escalations, clearer priorities, and less time spent chasing information.
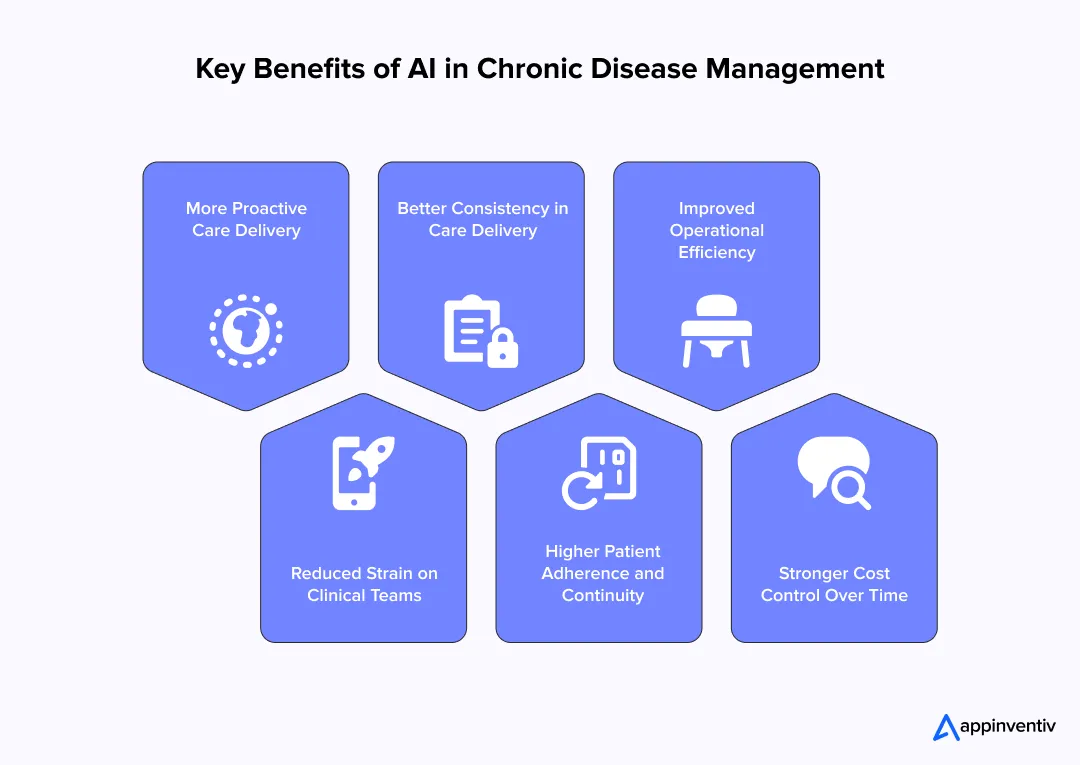
- More proactive care delivery: Instead of stepping in late, teams can act earlier. Small changes in patient data are detected sooner, helping prevent conditions from worsening.
- Reduced strain on clinical teams: Clinicians don’t have to dig through layers of data. They get a clearer view of what needs attention, making the workload easier to handle.
- Better consistency in care delivery: When everyone is working from the same signals, care becomes more uniform across teams and locations.
- Higher patient adherence and continuity: With tools such as AI-powered patient-monitoring apps, patients stay more engaged. Regular reminders and simple check-ins help keep care plans on track.
- Improved operational efficiency: Less manual follow-up and better prioritization mean teams can manage more patients without feeling stretched.
- Stronger cost control over time: Fewer emergency cases and smoother day-to-day operations make costs more predictable.
Over time, AI for chronic disease management helps things run more steadily. It’s not about perfection, but about making care easier to manage as patient volumes continue to grow.
Architecture for AI-Driven Chronic Disease Management
Spend a bit of time with a data engineering team, and the friction shows up quickly. One device sends readings ten minutes late, lab results come in a different format, and still, clinicians expect a clean, unified view on their screen. That’s where architecture quietly carries most of the load in AI-driven chronic care.
- Multi-source data ingestion with event handling: Data is coming from everywhere. EHRs, labs, wearables, patient apps. It rarely arrives in order. Teams rely on APIs and message queues to capture events as they occur, timestamp them, and handle delays or duplicates. This becomes especially important with remote monitoring, where signals can be inconsistent and timing matters.
- Data standardization and interoperability layers: Different systems often describe the same thing in completely different ways. Using standards like FHIR and HL7, teams map everything into a shared structure. Clinical vocabularies help preserve meaning. Without this layer, even well-built AI systems start producing outputs that are hard to trust.
- Hybrid processing for real-time and batch workloads: Not every signal needs an instant response. Some do. Streaming pipelines handle real-time alerts, while batch processing looks at trends, risk scores, and longer-term patterns. This split keeps things efficient without overengineering the system.
- AI/ML layer with lifecycle management: Models handle risk scoring, anomaly detection, and recommendations. But once they’re alive, the real work begins. Performance needs to be tracked, models retrained, and drift managed as patient behavior changes. That ongoing cycle is what keeps outputs reliable over time.
- Workflow integration and decision delivery: If insights sit in a separate tool, they get ignored. So teams push outputs directly into clinical decision support systems and existing dashboards. Clinicians don’t need raw data. They need clear, prioritized signals with next steps they can act on immediately.
- Security, compliance, and access control: This layer is non-negotiable. Data is encrypted, access is role-based, and every interaction is logged. As systems expand across departments or locations, this structure keeps things controlled and compliant without slowing teams down.
- Scalability and system resilience: Workloads fluctuate more than expected. Systems are built to scale on demand using containerized services and cloud infrastructure. That way, even during spikes or partial failures, the system stays available and responsive.
In more mature setups, this architecture is supported by an MLOps layer that manages model deployment, monitoring, and retraining cycles. Performance metrics, drift detection, and version control ensure models stay accurate as patient behavior and population health trends evolve. This becomes critical in AI in chronic disease management, where outdated models can lead to missed signals or unnecessary interventions.
Core Features of AI-Driven Chronic Disease Management Systems
In most enterprise setups, the problem isn’t collecting data. That part is already solved. The real challenge is making sense of it quickly and using it in a way that fits into how clinicians already work. That’s where the core features of AI in chronic disease management need to be practical, not just technically sound.
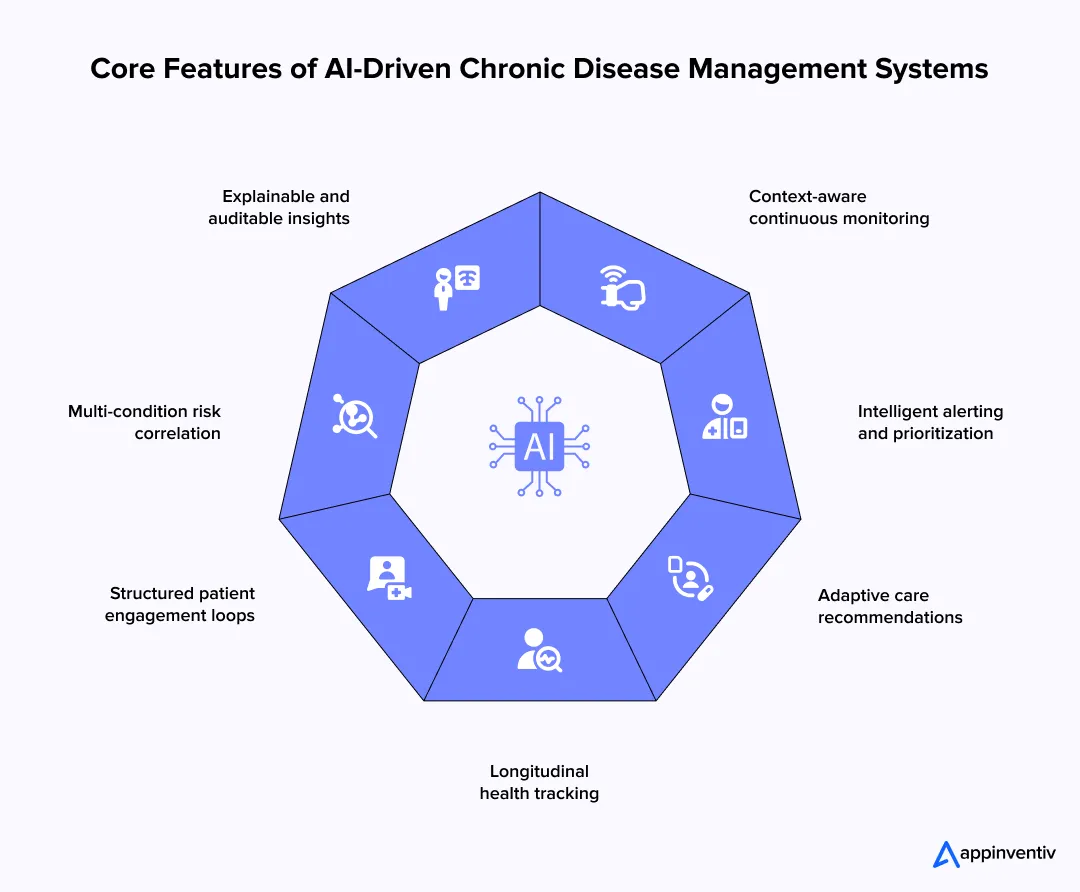
- Context-aware continuous monitoring: Data comes in from devices and AI patient monitoring systems, but raw numbers don’t tell the full story. The system must read this data in context. A change in vitals might be normal after activity but risky at rest. That layer of interpretation is what makes monitoring useful in day-to-day care.
- Intelligent alerting and prioritization: Care teams don’t have time to go through constant alerts. Strong systems filter signals based on patient history and trends, so only meaningful changes are surfaced. This keeps attention on what actually needs action and reduces alert fatigue.
- Adaptive care recommendations: Instead of fixed care plans, recommendations adjust as patient data changes. Using predictive analytics in chronic disease management, the system can suggest timely next steps, whether that’s a follow-up, a dosage change, or a closer review.
- Longitudinal health tracking: Most chronic conditions don’t change overnight. By tracking data over weeks and months, systems help identify slow declines or patterns that are easy to miss during routine visits.
- Structured patient engagement loops: Through AI patient monitoring apps, patients stay connected between visits. Regular inputs, reminders, and small feedback signals give care teams a better sense of adherence and emerging risks.
- Multi-condition risk correlation: Patients often deal with more than one condition at the same time. Systems connect those signals, allowing AI-based chronic disease monitoring systems to assess overall risk rather than examining each issue separately.
- Explainable and auditable insights: Clinicians need to understand why something is flagged. Instead of just showing a score, the system highlights contributing factors and trends. That clarity builds trust and makes decisions easier to validate.
When these features work well together, AI for chronic disease management doesn’t add complexity. It helps teams stay on top of patient health in a way that feels manageable and grounded in real workflows.
Also Read: AI in Medical Diagnosis for Speedy Healthcare Experience
Managing Data, Compliance, and Risk in AI-Driven Chronic Care Systems
This usually comes up right after a pilot starts showing results. The system works, early signals look promising, and then the harder questions begin. Where is the data coming from? Who can see it? What happens if something is wrong? In AI for chronic disease management, this is often the point at which teams decide whether they can scale with confidence.
- Data fragmentation and quality issues: Data is scattered across EHRs, labs, and AI patient-monitoring systems, and it rarely aligns perfectly. Missing entries, delays, or duplicates can easily affect outcomes. Teams deal with this early by cleaning, validating, and aligning data before it’s used.
- Privacy and compliance: It’s not just about meeting HIPAA or GDPR on paper. Systems need to hold up in real use. That means encryption, controlled access, and clear audit trails across AI healthcare disease management systems, so every data interaction is traceable.
- Secure data access and governance: Not everyone needs the same level of access. Clinicians, analysts, and admins all work differently. Role-based access keeps things controlled, while activity logs help maintain accountability.
- Model risk and explainability: When a patient is flagged as high risk, clinicians need to understand why. Clear reasoning behind outputs builds trust, and regular checks help ensure results stay accurate over time.
- Integration risks with legacy systems: Many older systems weren’t built to connect easily with newer digital health platforms. Careful API design and data mapping are needed to avoid gaps or delays in information flow.
When this layer is handled properly, teams feel more confident using the system. That’s what allows AI for chronic disease management to move from a controlled pilot into everyday use without hesitation.
Build AI Systems You Can Trust at Scale
Get the right foundation for secure, compliant, and reliable AI that holds up beyond pilot stages.
Future of AI in Chronic Disease Management
Spend a few minutes with a care team, and you’ll hear the same thing. They don’t want more tools. They want fewer surprises and a clearer sense of what’s happening between visits.
- Care becomes more continuous, not visit-based: Instead of waiting for the next appointment, changes get picked up as they happen. Teams can step in early, before issues become urgent.
- Better coordination across teams: Information won’t sit in separate systems as much. Teams will work from the same view, reducing the need for repeated checks and back-and-forth.
- Personalization becomes more natural: Care plans won’t stay fixed for long. As more data accumulates, they adjust in small, steady ways based on how the patient is actually doing.
- Closer link to everyday patient behavior: Data from wearable technology and daily routines start to matter more. Care feels less tied to clinic visits and more connected to real life.
- More automation in routine work: Reminders, basic follow-ups, and regular monitoring happen in the background. That frees up time for the cases that really need attention.
Over time, AI for chronic disease management becomes less visible as a separate layer. It just becomes part of how care runs: a bit steadier, a bit more predictable, and easier to manage as things grow.
As these systems evolve, the line between monitoring, decision-making, and care delivery continues to blur, with AI supporting everything from early detection to daily patient engagement and assisted care.
How Appinventiv Supports AI in Chronic Disease Management at Scale
You’ll notice the shift once a pilot starts gaining traction. What worked in a controlled setup now has to hold up inside real clinical systems, with constant data flow and day-to-day pressure from care teams.
Once AI moves beyond early experimentation, the challenge changes. It’s less about building models and more about making everything work together without slowing care.
That’s where Appinventiv steps in. As a software development company with strong healthcare experience, the team supports enterprises with practical AI consulting services that move initiatives from isolated use cases to scalable systems. The focus stays grounded. Start with the right problems, work with real-world data, and integrate AI into the tools clinicians already rely on.
Most of the complexity is handled behind the scenes, connecting EHRs, patient monitoring systems, and analytics layers so insights show up where decisions actually happen. In AI for chronic disease management, that integration is what drives adoption.
With 500+ digital health platforms, 450+ healthcare clients, and 75+ enterprise AI integrations, the approach is built for real environments, not just pilots.
If you’re planning to scale AI for chronic disease management, it helps to work with a team that understands how these systems behave in practice. Get Expert Consultation
FAQs
Q. How does AI improve chronic disease management
A. AI improves chronic disease management by continuously analyzing patient data from EHRs, monitoring devices, and historical records to detect early risk signals. This allows care teams to intervene sooner, reduce complications, and manage conditions proactively rather than reactively.
Q. How does AI help manage chronic diseases?
A. It helps teams stay connected to patients even when they’re not in the clinic. With AI healthcare care management systems, clinicians can track progress over time and step in when something looks off, rather than waiting for a scheduled check-in.
Q. What are common use cases for AI in chronic disease management?
A. Most organizations start with what’s practical. That usually means AI remote patient monitoring, identifying early risk, adjusting care plans, and using AI applications in diabetes management to manage specific conditions more closely.
Q. What technologies are used in AI healthcare monitoring systems?
A. Behind the scenes, it’s a mix of connected pieces working together. AI healthcare monitoring platforms, data pipelines, and machine learning models, combined with devices, run AI patient monitoring systems that track patient health in real time.
Q. What are the benefits of AI-driven chronic disease management?
A. You start to see fewer surprises. Patients are monitored more consistently, issues are caught earlier, and care teams can focus on what really needs attention. Over time, that leads to smoother day-to-day operations and better outcomes.
Q. How can healthcare organizations implement AI for chronic disease management?
A. Most teams don’t try to do everything at once. They start with one clear use case, make sure their data is in good shape, and then build or integrate an AI healthcare implementation for chronic care. Once it works, they expand gradually.
Q. How can Appinventiv support AI healthcare development?
A. Appinventiv works closely with teams to transform plans into working systems. From early discussions to deployment, the focus stays on building solutions that fit into real workflows and hold up as they scale.